- Request for Information (RFI): Evolving the Network of the National Library of Medicine
- Dental Therapists, Who Can Fill Cavities and Check Teeth, Get the OK in More States
- Colorectal Cancer Is Rising among Younger Adults. Some States Want to Boost Awareness.
- Rural Hospitals Built During Baby Boom Now Face Baby Bust
- Food Stamps Go Further in Rural Areas — Until You Add Transportation Costs
- CMS Announces Resources and Flexibilities to Assist with the Public Health Emergency in the State of Texas
- CMS Proposes New Payments for Digital Health Under CY2025 PFS Draft Rule
- Improving Public Health by Strengthening Community Infrastructure
- Biden Harris Administration Proposes Policies to Reduce Maternal Mortality, Advance Health Equity, and Support Underserved Communities
- Nearly Half of U.S. Counties Don't Have a Single Cardiologist
- Randolph County, Ill. Turns Unused Part of Nursing Home Into State-Of-The-Art Behavioral Health Center
- Safe and Stable Housing Is a Foundation of Successful Recovery
- Rural RPM Program Is a Lifeline for Pregnant Women
- Expert: Rural Hospitals Are Particularly Vulnerable to Increasing Cyberattacks Targeting Healthcare Facilities
- Biden-Harris Administration Invests Over $200 Million to Help Primary Care Doctors, Nurses, and Other Health Care Providers Improve Care for Older Adults
COVID-19 Death Rates in Urban and Rural Areas.
 The latest data from the Centers for Disease Control and Prevention show that, in 2020, deaths due to COVID-19 became the third leading cause of death in the United States. The death rate that year was highest in most urban areas at 97.7 deaths per 100,000 people. But the second-highest rate of death was in the most rural areas at 90.6 deaths per 100,000 people. Among males under age 65, those in the most urban areas had the highest COVID-19 death rates; among females, rates were highest in the most rural areas.
The latest data from the Centers for Disease Control and Prevention show that, in 2020, deaths due to COVID-19 became the third leading cause of death in the United States. The death rate that year was highest in most urban areas at 97.7 deaths per 100,000 people. But the second-highest rate of death was in the most rural areas at 90.6 deaths per 100,000 people. Among males under age 65, those in the most urban areas had the highest COVID-19 death rates; among females, rates were highest in the most rural areas.
CMS Finalizes Medicare Policies for ACOs
CMS also released the Physician Fee Schedule final rule for the calendar year 2023 this week, addressing new policies for Accountable Care Organizations (ACOs) in the Medicare Shared Savings Program that support providers treating rural and underserved populations. The final includes updates to policies on evaluation/management services, telehealth services, behavioral health services, and Opioid Treatment Programs. Additionally, CMS incorporated new chronic pain management and behavioral health integration services to the Rural Health Clinic and Federally Qualified Health Center specific general care management HCPCS code, G0511.
CMS Finalizes Medicare Policies for Rural Emergency Hospitals
 This week, the Centers for Medicare & Medicaid Services (CMS) released the final payment policies for the Medicare Hospital Outpatient Prospective Payment System for the calendar year 2023. This rule also includes payment, enrollment, and conditions of participation policies for the new provider type, Rural Emergency Hospitals. Finally, CMS is codifying in regulation the location and distance requirements that Critical Access Hospitals (CAHs) must meet for certification, including a new definition for “primary road’ used for determining the driving distance of a CAH and its proximity to other providers. FORHP is funding technical assnam10.safelinks.protection.outlook.comistance to support rural hospitals exploring the Rural Emergency Hospital option.
This week, the Centers for Medicare & Medicaid Services (CMS) released the final payment policies for the Medicare Hospital Outpatient Prospective Payment System for the calendar year 2023. This rule also includes payment, enrollment, and conditions of participation policies for the new provider type, Rural Emergency Hospitals. Finally, CMS is codifying in regulation the location and distance requirements that Critical Access Hospitals (CAHs) must meet for certification, including a new definition for “primary road’ used for determining the driving distance of a CAH and its proximity to other providers. FORHP is funding technical assnam10.safelinks.protection.outlook.comistance to support rural hospitals exploring the Rural Emergency Hospital option.
631 Rural Hospitals at Risk of Closure, by State
Across the U.S., a total of 631 rural hospitals — or about 30 percent of all rural hospitals — are at risk of closing in the immediate or near future due to persistent financial losses on patient services, inadequate revenues to cover expenses, and low financial reserves, according to a report from the Center for Healthcare Quality and Payment Reform.
More than 200 of the rural hospitals in the report are identified as being at immediate risk of closure. These hospitals were losing money on patient services before the COVID-19 pandemic, and they did not have sufficient resources to cover those losses, according to the report. Click here to view the numbers and percentage of rural hospitals by state at risk as of October 2022, based on the Center for Healthcare Quality and Payment Reform analysis.
Rural Adults have Lower Rates of Employer Sponsored Health Insurance in Pennsylvania
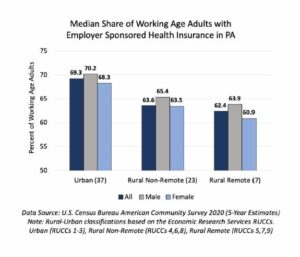 The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
The Penn State Rural Health Disparities Lab in the Department of Biobehavioral Health has released a report showing rates of employer-sponsored health insurance in rural Pennsylvania. Employer sponsored health insurance (ESHI) is typically subsidized by employers, which can reduce the overall cost for employees. Using data from the American Community Survey, we found that working-age adults living in rural areas in Pennsylvania are less likely to have ESHI than those in urban areas. Across all rural-urban categories, females were least likely to have ESHI. The lower rates in rural areas may reflect fewer job opportunities with established ESHI plans. These findings raise concerns about access to the benefits of ESHI in rural contexts, especially for females. Author: Melanie Dececco, RHO Undergraduate Research Assistant
Apply for the HIV & Aging Scholars Program by Nov. 3
Applications are open for the second cohort of the HIV & Aging Scholars Program. This is an interprofessional program open to individuals from any discipline (nursing, social work, pharmacy, medicine, physical therapy, etc.) and people aging with HIV, advocates, peer navigators, case managers, and others from community organizations. Using a cohort-based model, selected candidates will participate in a six-month virtual learning community with national experts and mentors with the goal of improving HIV & aging services in local communities and clinical or community-based settings. Participants will be eligible for CNE and other benefits. View the cohort 1 participants and their projects! Applications for the second cohort are due Nov. 3. Learn more about the program and how to apply.
Pennsylvania Behavioral Health Telehealth Phase II Roadmap is Released
The Office of Mental Health and Substance Abuse Services (OMHSAS) is pleased to share the Pennsylvania Behavioral Health Telehealth Phase II Roadmap, which was developed in collaboration with the OMHSAS Telehealth Steering Committee and Mercer Government Services Consulting. This report focuses on identifying and prioritizing recommendations for short-term and long-term implementation of telehealth services in the Commonwealth. The roadmap includes example documents developed by the Steering Committee that can be used and personalized by the provider when implementing telehealth services. The work of the Steering Committee and other stakeholders has been and will continue to be vital in ensuring that the behavioral health needs of Pennsylvanians continue to be met.
Research Study Shows that Workers are Less Engaged but Still Working Hard
According to a Conference Board survey, 30% of workers say their level of engagement at work—the commitment and connection that employees feel to their work—is lower than six months ago. Lower engagement, however, isn’t necessarily affecting effort: Only 18% say their level of effort has decreased in the last six months. Fifty percent say it’s the same; 31% say it’s increased.
The New Pandemic: Loneliness
Loneliness in America is widespread — and it’s a public health problem. According to a Harvard study, more than one in three Americans are lonely. That rises to 61% when looking at younger people, and 51% among mothers with young kids. Read more.
Nearly 334,000 Providers Left the Healthcare Workforce in 2021
Modern Healthcare reported on Oct. 20, 2022, that nearly 334,000 providers left the healthcare workforce in 2021, driven by burnout and concerns related to the pandemic, according to a report by Definitive Healthcare. About 117,000 were physicians, 53,000 were nurse practitioners, and nearly 23,000 were physician assistants. Read more.
