- Request for Information (RFI): Evolving the Network of the National Library of Medicine
- Dental Therapists, Who Can Fill Cavities and Check Teeth, Get the OK in More States
- Colorectal Cancer Is Rising among Younger Adults. Some States Want to Boost Awareness.
- Rural Hospitals Built During Baby Boom Now Face Baby Bust
- Food Stamps Go Further in Rural Areas — Until You Add Transportation Costs
- CMS Announces Resources and Flexibilities to Assist with the Public Health Emergency in the State of Texas
- CMS Proposes New Payments for Digital Health Under CY2025 PFS Draft Rule
- Improving Public Health by Strengthening Community Infrastructure
- Biden Harris Administration Proposes Policies to Reduce Maternal Mortality, Advance Health Equity, and Support Underserved Communities
- Nearly Half of U.S. Counties Don't Have a Single Cardiologist
- Randolph County, Ill. Turns Unused Part of Nursing Home Into State-Of-The-Art Behavioral Health Center
- Safe and Stable Housing Is a Foundation of Successful Recovery
- Rural RPM Program Is a Lifeline for Pregnant Women
- Expert: Rural Hospitals Are Particularly Vulnerable to Increasing Cyberattacks Targeting Healthcare Facilities
- Biden-Harris Administration Invests Over $200 Million to Help Primary Care Doctors, Nurses, and Other Health Care Providers Improve Care for Older Adults
FCC: Promoting Telehealth for Low-Income Consumers; COVID-19 Telehealth Program
Apr 9, 2020 — The Federal Communications Commission has released a rule to establish the COVID-19 Telehealth Program and the Connected Care Pilot Program. The COVID-19 Telehealth Program provides $200 million for healthcare providers to provide connected care services to patients in their homes or mobile locations in response to the COVID-19 pandemic. This program is effective April 9, 2020. The Connected Care Pilot Program will provide up to $100 million over three years to examine how the Universal Service Fund can support the trend toward connected care services to consumers, particularly for low-income and veteran populations. The Connected Care Pilot Program will be effective once approved by the Office of Management and Budget. Read more here.
HHS, CDC: Approval Tests and Standards for Air-Purifying Particulate Respirators
Apr 14, 2020 — Notice of interim final rule with comment period to update the regulatory requirements used by the National Institute for Occupational Safety and Health (NIOSH) to test and approve air-purifying particulate respirators for use in the ongoing COVID-19 pandemic. The rule will be effective April 14, 2020. Comments are due by August 12, 2020. Read more here.
COVID-19 Resources for Non-English-Speaking People
The COVID-19 Health Literacy Project provides translations of essential information about COVID-19 in more than 35 languages. Harvard faculty has vetted all of the information in this project that was started by a medical student at Harvard. Patients with limited English proficiency are likely to be at higher risk for COVID-19 and its complications. These translational materials, along with a guidance article, Culturally and Linguistically Competent Care from ECRI, can help provide health centers with the information needed to communicate with those patients whose first language is not English and other patients with diverse cultural needs.
Contact Tracing – Guidance on this Path Out of Isolation
Contact tracing is what is now on everyone’s radar in order to help in the next step to begin to open up the country. Contact tracing is a process designed to halt the chain of transmission of an infectious pathogen–like the coronavirus–and slow community spread. When someone tests positive for an infectious disease, they become a “case.” Public health workers then reach out to the case to make sure they have what they need and that they are self-isolating. They will then figure out who they had contact with who may be at risk of infection, too. NPR recently released a guide on the basics of the process and how it might help society restart after the current wave of coronavirus cases.
US’s digital divide ‘is going to kill people’ as Covid-19 exposes inequalities
Amanda Holpuch, The Guardian
Exclusive research shows drop in connectivity is impacting rural and urban areas with populations already underserved by the medical system or racked with poverty
The Covid-19 crisis is exposing how the cracks in the US’s creaking digital infrastructure are potentially putting lives at risk, exclusive research shows.
With most of the country on lockdown and millions relying on the internet for work, healthcare, education and shopping, research by M-Lab, an open source project which monitors global internet performance, showed that internet service slowed across the country after the lockdowns.
“This is going to kill people,” said Sascha Meinrath, co-founder of M-Lab.
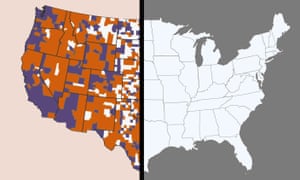
In late March, most people in 62% of counties across the US did not have the government’s minimum download speed for broadband internet, according to M-Lab.
Between February and mid March, when the pandemic was only just beginning to hit the US, there was a 10% increase in how many counties saw download speeds fall below the government standard, representing about one in 10 US counties, M-Lab found.
“Now that people’s livelihoods, schools and lives, are literally on the line, we can’t survive,” Meinrath said. “These communities that are underserved are not going to be able to transition to an online workplace or school environment.”
Summary of Medicare Emergency COVID-19 Waivers for Health Care Providers
CMS has temporarily waived several Medicare regulations to support hospitals, clinics, and other healthcare facilities during the 2019 Novel Coronavirus (COVID-19) pandemic. The new waivers focus on reducing supervision and certification requirements so that practitioners can be hired quickly and perform work to the fullest extent of their licenses. This Fact Sheet summarizes the new changes in addition to previous waivers that impact all types of providers, including Critical Access Hospitals, Rural Health Clinics, physicians, skilled nursing facilities, and others.
Rural Response to Coronavirus Disease 2019
The Rural Health Information Hub has created a guide to help you learn about activities underway to address COVID-19. Find more information here.
Confirmed COVID-19 Cases, Metropolitan and Nonmetropolitan Counties
The RUPRI Center for Rural Health Policy Analysis provides up-to-date data and maps on rural and urban confirmed cases throughout the United States. Find data briefs here. An animated map shows the progression of cases beginning January 21.
NCSL on COVID-19: Health Care in Rural America
The National Conference of State Legislatures (NCSL) focuses on rural areas in its podcast about state-level response to the pandemic. Find the podcast here.
RAND: Responding to Critical Care Surge Capacity
The RAND Corporation (Research ANd Development) included 61 rural hospitals in its survey of hospitals across the country about their capacity to respond to the Coronavirus pandemic. The report presents a range of strategies for creating capacity, including an online Critical Care Surge Response Tool that allows decision-makers at all levels — hospitals, health care systems, states, regions — to estimate current critical care capacity and rapidly explore strategies for increasing it. Read more here.
